When you're looking at a wound that just won't heal, one of the most common culprits is slough. It’s the stringy, yellowish, or tan gunk that can cover part or all of the wound bed. But it’s more than just an unpleasant sight—it's a roadblock to recovery.
Think of it as biological debris. Slough is a stubborn mix of dead cells, fibrin, and cellular waste that physically blocks the growth of new, healthy tissue. Its presence is a clear signal that the wound is stuck. For clinicians, understanding how to effectively assess and manage this barrier is a cornerstone of advanced wound care. Failure to address slough means prolonged healing times, increased patient discomfort, and a higher risk of serious complications. This guide provides a comprehensive framework for tackling slough, from initial identification to advanced management strategies.
What Is Slough and Why Does It Stall Healing?
Imagine trying to build a new house on a foundation cluttered with old, decaying materials. You can't. The same principle applies to wound healing. For the body to build new granulation tissue—the healthy, red, bumpy tissue that fills a wound—it needs a clean, clear surface.

Slough essentially smothers the wound bed. This accumulation of devitalized tissue shows that the body's natural cleanup crew is overwhelmed, keeping the wound locked in a state of chronic inflammation. The healing process simply can't move forward. The presence of slough indicates that the wound has failed to transition from the inflammatory phase to the proliferative phase of healing. It perpetuates a cycle of cellular stress and prevents the necessary signaling for tissue reconstruction.
The Clinical Significance of Slough
Dealing with slough in a wound bed isn't just about tidying up. It's a critical clinical intervention with direct consequences for your patient. Here’s why it demands your immediate attention:
- It Fuels Inflammation: Slough acts as a foreign body, triggering a constant inflammatory response that prevents the wound from progressing to the next stage of healing. This prolonged inflammation can lead to further tissue damage and pain.
- It’s a Buffet for Bacteria: This dead tissue is a perfect nutrient source for bacteria, encouraging colonization and biofilm formation, which significantly increases the risk of infection. Biofilms are particularly insidious, creating a protective matrix that makes bacteria resistant to antibiotics and the host's immune system.
- It Hides the Real Problem: A thick layer of slough makes it impossible to see what's really going on underneath. You can't accurately measure the wound, assess its true depth, or check for exposed bone or tendon. This masking effect can lead to missed diagnoses of underlying issues like osteomyelitis or deep tissue injury.
A wound covered in slough is a wound that cannot heal. Removing this barrier is the first and most essential step in restarting the healing cascade and moving a chronic wound toward closure.
The urgency here can't be overstated. Research highlights slough as a major obstacle, with some studies showing it can cover over 70% of the wound bed in many chronic cases. To learn more, you can read the full research about these findings on wound management. This guide is designed to give you evidence-based strategies to assess and manage slough, helping you turn a stalled wound into one that has a clear path to recovery.
Slough Characteristics At A Glance
To effectively treat slough, you first need to identify it correctly. It can sometimes be confused with other tissues, but its specific characteristics provide clear clues. Correct identification is fundamental to selecting the appropriate debridement method and dressing, preventing iatrogenic harm from mismanaging healthy tissue.
This table provides a quick reference to help you identify slough during a wound assessment.
| Characteristic | Description | Clinical Implication |
|---|---|---|
| Color | Typically yellow, tan, gray, or greenish. Can be white. | Color can indicate the level of hydration and bacterial load. A greenish tint may suggest a pseudomonas infection. |
| Texture | Can be stringy, fibrinous, gelatinous, or thick and leathery. | Texture helps determine the best debridement method. Stringy slough may be easier to remove than thick, adherent slough. |
| Adherence | May be loosely attached in clumps or firmly adhered to the wound bed. | Tightly adhered slough is more difficult to remove and often requires more aggressive debridement techniques. |
| Amount | Can be minimal (less than 25%) or extensive (covering the entire wound bed). | The percentage of slough coverage is a key indicator of healing progress and must be documented accurately. |
| Odor | Often has a mild, non-specific odor, but a foul smell suggests infection. | A change in odor is a red flag for infection and warrants further investigation, such as a wound culture. |
Recognizing these features is the first step in creating an effective plan of care. The more accurately you can describe the slough, the better you can tailor your treatment strategy. Detailed assessment and documentation are not just best practices; they are a clinical necessity for effective wound management.
How to Accurately Assess Wound Slough
Managing a wound with slough effectively all starts with a precise, systematic assessment. Think of it like a detective arriving at a crime scene—you can't solve the case with just a quick glance. You have to meticulously gather clues. In the same way, clinicians need to evaluate the wound bed in detail to choose the right treatment path.
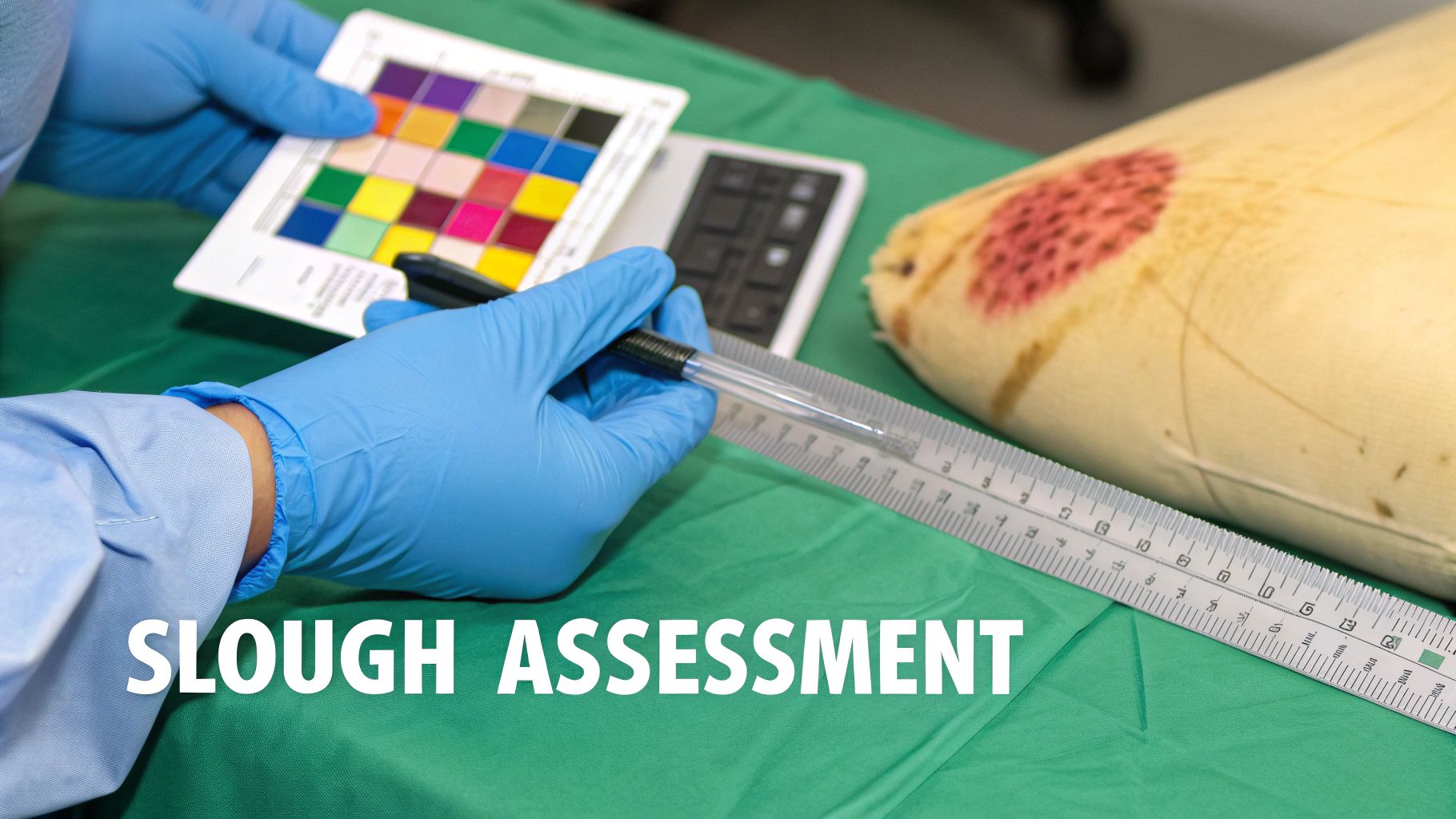
This thorough evaluation isn’t just about ticking a box; it creates a crucial baseline. Without it, you can't track progress or justify your clinical decisions. Treatment becomes guesswork, which can easily delay healing or, worse, cause harm. A robust initial assessment provides the data needed to create a care plan and serves as the benchmark against which all future assessments are compared.
Quantifying Slough Coverage
Your first move is to figure out just how much of the wound bed is covered by slough. We typically document this as a percentage. It helps to visualize the wound bed as a pie chart. What slice of that pie is slough, and what slice is healthy granulation tissue or something else?
This simple measurement is a powerful tool for tracking progress. For example, if a wound goes from 80% slough coverage down to 50% over a couple of weeks, that’s a clear win. It shows your treatment is working, even if the wound's overall size hasn't shrunk yet. This objective metric is invaluable for demonstrating treatment efficacy to patients, colleagues, and insurance payers.
Decoding the Visual Cues of Slough
Once you have the amount, it’s time to look closer at the quality of the slough. Its appearance provides a wealth of information about the wound’s environment, from its hydration level to the bacterial bioburden.
Pay close attention to three key characteristics:
- Color: Most of the time, slough is yellow or tan. But it can also show up as grayish or off-white. If you see a greenish tint, that's a major red flag—it often points to a Pseudomonas infection, which can carry a distinctive "fruity" odor.
- Consistency: The texture tells a story. It can be thin and stringy or thick and gelatinous. This information directly guides your debridement choices. Loosely attached, stringy slough might come off with gentle methods, whereas thick, dense slough is going to require a more aggressive approach.
- Adherence: Is the slough loosely clumped on the surface, or is it stuck fast to the wound bed? Tightly adherent slough is much tougher to remove and creates a stubborn roadblock to healing. The level of adherence dictates the intensity of the debridement needed and can impact patient comfort during the procedure.
Documenting these specifics is key. A note like, "Wound bed is approximately 60% covered in adherent, yellow, gelatinous slough," paints a clear, reproducible picture for the next clinician who sees the patient.
Differentiating Slough from Other Tissues
Here’s where even experienced clinicians can get tripped up. One of the biggest challenges in wound assessment is telling slough apart from other tissues that can look deceptively similar. A misidentification can lead you down the wrong treatment path, like trying to remove healthy tissue or leaving non-viable tissue behind.
Here’s a quick guide to telling the common look-alikes apart:
| Tissue Type | Key Differentiators | Clinical Action |
|---|---|---|
| Slough | Yellow, tan, or gray; can be stringy or gelatinous; indicates stalled healing and non-viable tissue. | Must be removed through debridement to let healing move forward. |
| Fibrin | Thin, stringy, and often yellowish-white; a normal part of the early clotting and healing process. | Generally should not be aggressively removed, as it provides a scaffold for new tissue. |
| Eschar | Black or brown, dry, and leathery; represents full-thickness tissue death. | Requires debridement, though stable eschar on a heel may be left intact. |
This systematic approach—quantifying the amount, analyzing the characteristics, and distinguishing it from other tissues—is the bedrock of effective wound care. It ensures your interventions are targeted and your documentation is crystal clear. For those looking to sharpen their evaluation skills, exploring advanced wound assessment tools for nurses can offer additional support for consistent and accurate documentation. Mastering this process turns wound assessment from a subjective glance into an objective, data-driven skill that has a direct impact on patient outcomes.
Choosing the Right Debridement Strategy
Once you’ve sized up the amount and type of slough in a wound, the next move is clear: you have to get it out. This process, called debridement, is completely non-negotiable if you want the wound to heal. It is a fundamental principle of wound bed preparation, aimed at removing necrotic tissue, foreign material, and bacterial biofilms.
Think of it like clearing a cluttered construction site. You can't lay a new foundation until all the debris is gone. The same principle applies here.

Picking the right debridement method isn't a one-size-fits-all decision. It's a clinical judgment call that balances the wound's needs, the patient's overall condition, and the resources you have on hand. The goal is always to remove that non-viable tissue while protecting the healthy, viable tissue right underneath it. Key factors in this decision include the patient's pain tolerance, the presence of infection, vascular status, and the clinician's skill level.
Comparing Debridement Methods For Slough Removal
To make the best choice, it helps to see the different debridement methods side-by-side. Each has its own strengths and is suited for different clinical situations. This table breaks down the most common options to help guide your decision-making at the bedside.
| Debridement Method | Mechanism | Best For | Considerations |
|---|---|---|---|
| Autolytic | The body's own enzymes break down non-viable tissue in a moist environment. | Stable, non-infected wounds with minimal to moderate slough. | Slowest method; requires a patient with a functioning immune system. Not for infected wounds. |
| Enzymatic | A topical agent (like collagenase) is applied to selectively dissolve slough. | Patients who can't tolerate sharp debridement; good for softening thick, adherent eschar/slough. | Requires a prescription and daily application. Can be costly. |
| Mechanical | Physical force removes slough (e.g., irrigation, monofilament pads, wet-to-dry dressings). | Wounds with loosely adherent slough and debris. | Can be non-selective and may damage healthy tissue. Wet-to-dry dressings are often painful. |
| Sharp | A trained clinician uses sterile instruments (scalpel, curette) to precisely cut away slough. | Thick, adherent slough and eschar; when rapid debridement is needed. | The gold standard for speed and efficiency. Requires specific training, skills, and licensure. |
Ultimately, selecting the right tool for the job depends on a thorough wound assessment. A combination approach is often the most effective way to prepare the wound bed for healing. For instance, enzymatic agents can soften slough, making it easier to remove later with conservative sharp debridement.
Autolytic Debridement: Letting the Body Do the Work
Autolytic debridement is the most selective and gentle approach on the list. It’s all about creating the right conditions for the body to use its own enzymes and immune cells to dissolve slough. The key is maintaining a moist wound environment.
To make this happen, you’ll turn to moisture-retentive dressings. These trap the wound's natural fluids, putting those enzymes right to work.
- Hydrogels: Perfect for drier wounds that need a little moisture donated to the wound bed. They rehydrate necrotic tissue, facilitating its separation.
- Hydrocolloids: Great for wounds with light to moderate drainage, as they form a gel that keeps the area moist.
- Transparent Films: Best for wounds with very little exudate, sealing in moisture to kickstart autolysis.
Autolytic debridement is a slow and steady process. It’s the go-to for stable wounds in patients who aren't immunocompromised and show no signs of infection.
Enzymatic Debridement: A Targeted Chemical Assist
Sometimes, the body’s natural process needs a little nudge. That's where enzymatic debridement comes in. This method uses a prescribed topical agent containing enzymes that specifically target and break down non-viable tissue.
The most common enzyme used is collagenase. It works by digesting the collagen fibers that anchor slough to the wound bed. This chemical action is incredibly precise, detaching the gunk without harming the healthy granulation tissue underneath. It’s an excellent option for patients who can't handle more aggressive methods or when sharp debridement isn't an option. It can also be used in conjunction with other methods to enhance their effectiveness.
Mechanical Debridement: The Physical Approach
As the name suggests, mechanical debridement involves physically removing slough. While it can be effective, it’s also non-selective, which means it can accidentally take healthy tissue along with the bad stuff. For this reason, some older methods are used much more cautiously today.
Here are a few common techniques:
- Wet-to-Dry Dressings: Once a go-to, this method is now used with care. A wet gauze dries in the wound and is then pulled away, taking tissue with it. It can be painful and traumatic to new tissue.
- Wound Irrigation: Using pressurized saline to flush the wound is a much gentler form of mechanical debridement. It's great for washing away loose slough and debris.
- Monofilament Pads: These special pads have a textured surface designed to gently lift slough from the wound bed when wiped across it.
Sharp Debridement: The Gold Standard for Speed
When you need to get rid of thick, stubborn slough quickly, nothing beats sharp debridement. This is a procedure performed by a trained clinician using sterile tools—like a scalpel, curette, or scissors—to literally cut away the non-viable tissue.
There are two main categories:
- Conservative Sharp Debridement: This is typically done at the bedside. The clinician removes only the devitalized tissue that is clearly identifiable, often without needing anesthesia.
- Surgical Debridement: This is a more extensive procedure done in an operating room, usually with anesthesia. It's reserved for wounds with a large amount of slough, signs of infection, or when a deeper exploration is needed.
Having a solid grasp of these options allows you to build a truly effective care plan. For example, managing a complex pressure injury often involves using several of these techniques in combination. You can see how debridement fits into a larger strategy in our detailed guide on stage 3 decubitus ulcer treatment. Making the right choice means you’re removing barriers to healing, not accidentally creating new ones.
Selecting Dressings to Manage Slough and Exudate
Once you’ve decided on a debridement strategy, the job isn’t done. Far from it. Choosing the right dressing is an active, ongoing part of managing slough in the wound bed. A dressing is so much more than a simple cover; it’s a critical tool that helps you create the perfect healing environment, supports your debridement efforts, and stops slough from coming right back.
Think of it like tending a garden. After you’ve meticulously pulled all the weeds (debridement), you lay down the right kind of mulch (dressing). This keeps new weeds out, holds in just the right amount of moisture, and gives your plants the best shot at thriving. The wrong dressing can either drown the wound in too much fluid or dry it out completely—and both scenarios will stall healing and roll out the welcome mat for more slough.
Matching Dressing Function to Wound Needs
Picking a dressing isn't about brand loyalty; it's about matching its function to what the wound needs right now. A dressing that's a perfect fit today might be the wrong choice a week from now as the wound changes. The key is to constantly reassess the wound bed, paying close attention to two main factors: the moisture level (exudate) and the kind of slough you're dealing with.
To simplify things, you can think of dressings in terms of their primary job:
- Donating Moisture: These are your go-to for dry, dehydrated wounds where the slough is thick and leathery.
- Absorbing Moisture: You'll need these for wounds with moderate to heavy drainage to stop the surrounding skin from getting waterlogged and breaking down.
- Managing Bioburden: These become essential when you suspect a high bacterial load or infection hiding within the slough.
The goal is always to strike a perfect moisture balance. A wound bed that is moist—but not wet—is the ideal environment for the body’s own enzymes to keep breaking down any leftover slough through autolytic debridement.
The presence of slough is a major red flag for infection risk and healing delays. In fact, research shows that over 75% of non-healing wounds contain biofilm mixed in with slough. Following a clear, evidence-based pathway that includes thoughtful dressing selection really works. For example, one wound initially covered in slough improved to just 30% slough and 70% granulation tissue. The patient's pain dropped to zero, and the wound nearly healed, all thanks to consistent weekly reassessments and proper care. You can discover more insights about implementing an evidence-based pathway for non-healing wounds.
Dressings That Promote Autolytic Debridement
For wounds that are on the drier side or have minimal drainage, your main goal is to add or conserve moisture. This gives the body’s natural debridement process a helping hand.
- Hydrogels: These are water or glycerin-based gels and sheets that actively donate moisture to a parched wound bed. They are fantastic for softening up hard, desiccated slough, which makes it much easier to remove later.
- Hydrocolloids: These dressings create a gel as they interact with wound fluid, forming a moist, sealed environment. They work best for wounds with low to moderate exudate and have the added benefit of being wearable for several days.
Dressings That Absorb Heavy Exudate
Now for the other end of the spectrum: wounds that produce a lot of fluid. When exudate is out of control, it can easily damage the healthy skin around the wound, creating a soupy mess where bacteria love to multiply.
- Calcium Alginates: Made from seaweed, these are incredibly absorbent dressings, capable of soaking up to 20 times their own weight in fluid. They transform into a soft gel within the wound, which traps exudate and debris while still keeping the wound bed moist.
- Foams: Foam dressings are absorbent powerhouses that also provide a soft, protective cushion. They're a great choice for managing moderate to heavy exudate and come in all sorts of shapes and sizes to fit just about any wound.
Dressings That Manage Bioburden
When you suspect a high bacterial load or see early signs of a localized infection, an antimicrobial dressing is your best ally. These dressings are infused with agents like silver, iodine, or medical-grade honey.
Their job is to reduce the number of microorganisms in the wound bed, which helps get inflammation under control and stops slough from becoming an incubator for infection. Just remember to use them judiciously and only when there’s a clear clinical need to avoid contributing to microbial resistance. By choosing a dressing thoughtfully, you're not just covering a wound—you are actively steering it toward healing.
Improving Documentation for Slough Management
Great clinical care falls flat without the documentation to back it up. When you're managing slough in a wound bed, precise charting is much more than an administrative chore—it's essential for patient safety, seamless care transitions, and getting paid for your work. Vague notes simply don't justify the medical necessity of your interventions, which can lead to frustrating claim denials and dangerous communication gaps between care teams.
Think of your documentation as telling the wound's story. It needs to paint a vivid picture of the wound’s condition and clearly explain the complex care it requires. Just writing "slough present" doesn't cut it. Strong documentation provides the specific, objective details that auditors and payers need to see to approve treatments like debridement or advanced dressings.
Crafting Precise and Defensible Charting Notes
To create documentation that holds up under scrutiny, your notes need to be objective, detailed, and consistent. The goal is to show, not just tell. Ditch the subjective terms and instead lean on quantifiable data and descriptive language that another clinician could easily pick up and understand.
Here are the key details to include every time you document a wound with slough:
- Percentage of Slough: Estimate the amount of the wound bed covered in slough (e.g., "50% slough"). This is one of the most important metrics for tracking whether the wound is getting better or worse.
- Slough Characteristics: Describe its appearance and feel. Note the color (yellow, tan, green), its consistency (is it stringy or more gelatinous?), and how firmly it's attached (loosely attached vs. firmly adherent).
- Justification for Treatment: This is where you connect the dots. Clearly explain why the slough necessitates a specific intervention. Why did you choose that particular debridement method or dressing?
Example of weak documentation: "Wound has some slough. Cleaned and dressed."
Example of strong documentation: "Wound bed is covered with approximately 70% firmly adherent, thick, yellow slough, preventing assessment of the wound base. Conservative sharp debridement is medically necessary to remove this non-viable tissue barrier and promote granulation."
See the difference? This level of detail validates your clinical judgment and builds an undeniable case for reimbursement. It tells a complete clinical story, protecting both the patient and the provider.
Navigating Relevant Coding and Reimbursement
Your detailed documentation is the bedrock of proper coding. In wound care, specific codes are the language used to communicate the patient's diagnosis and the services you provided. A mismatch between your clinical notes and the codes you submit is a fast track to a denied claim.
Get comfortable with the main code sets for managing wounds with slough:
- ICD-10-CM Codes: These are the diagnosis codes. You’ll use codes that identify the underlying wound type (like a pressure ulcer or venous ulcer) and can add secondary codes to specify the presence of slough or necrosis.
- CPT Codes: These codes describe what you actually did. For slough, debridement codes (97597, 97598) are your go-to. Your notes absolutely must support the use of these codes by detailing the depth of tissue you removed and the instruments you used.
When your clinical charting and coding are in sync, you ensure the complexity of your care is accurately captured. This not only supports your facility’s revenue cycle but also solidifies the plan of care for the next clinician. To make this process more consistent, using a structured wound care documentation template can be a game-changer, providing a clear framework to capture all the essential details every single time.
How AI Is Transforming Wound Care Workflows
For years, managing slough in a wound bed has been a subjective and time-consuming process. We’ve relied on visual assessments and then faced a mountain of paperwork to document what we saw. While this is the standard of care, it often leads to inconsistencies and pulls clinicians away from their patients.
Now, technology is stepping in to solve these exact problems. AI-powered platforms are making wound care workflows faster, more accurate, and far less of a headache. The integration of artificial intelligence is not just an incremental improvement; it is a paradigm shift in how we approach wound assessment and documentation.
Automating Assessment for Objective Insights
Let’s be honest: the human eye is skilled, but it’s also subjective. One clinician might estimate 20% slough, while another sees 30%. That variability can make it tough to consistently track healing. AI takes the guesswork out of the equation.
By analyzing a simple digital photo of the wound, these systems can instantly calculate:
- Wound Dimensions: Precise length, width, and surface area without a ruler.
- Tissue Percentage: The exact percentage of slough, granulation, and eschar is quantified automatically.
- Healing Trajectory: The platform tracks these changes over time, giving you a clear, data-driven picture of how the wound is progressing.
This isn’t some far-off concept; it’s happening right now. A tool like Ekagra Health AI can analyze and segment a wound image with a single click.

This level of detail creates an objective baseline. It means the entire clinical team can make more informed decisions based on consistent, reliable data instead of subjective estimates. This objectivity strengthens clinical communication, improves research data quality, and provides irrefutable evidence for reimbursement.
From Voice to Claim: Making Documentation Disappear
Beyond assessment, the biggest win with AI is in documentation. The administrative burden of charting is a massive contributor to clinician burnout. We’ve all felt it. Reducing that time spent on paperwork directly improves both job satisfaction and the quality of patient care.
Think about capturing all your observations and notes just by speaking during the patient visit. Voice-to-chart technology does exactly that. The AI listens, transcribes everything into a structured and compliant chart note, and even maps it to the correct ICD-10 and CPT codes.
This single feature can shrink the documentation workflow from hours down to minutes. By handling the heavy lifting of charting and coding, AI frees up our most valuable resource: time. It allows us to shift our focus from the keyboard back to our patients, ensuring every decision is backed by accurate, consistent data. This technological leap promises a future where clinicians are empowered to practice at the top of their license, unburdened by administrative tasks.
Got Questions About Slough? We've Got Answers.
When you're dealing with complex wounds, you're bound to run into questions, especially about something as stubborn as slough. Here are some quick, clear answers to the questions we hear most often from fellow clinicians, designed to help you make confident calls right at the bedside.
Is Slough a Sign of Infection?
It can be a major red flag. While slough itself is just dead tissue, its presence is a huge risk factor for infection. Think of it as a standing invitation for bacteria to move in and set up shop.
Pay close attention to any changes. A sudden increase in the amount of slough, a shift in color towards green, or a new, foul odor are all warning signs. Slough creates a perfect breeding ground for bacteria to thrive and build resilient biofilms. If you see these signs, it's time to look closely for other classic signs of infection—like more pain or spreading redness—and consider reaching for an antimicrobial dressing to get that bioburden under control.
How Often Should a Sloughy Wound Be Debrided?
There’s no one-size-fits-all answer here; it really depends on the wound itself, how much slough is in the wound bed, and the debridement method you've chosen.
- Autolytic Debridement: This is a slow and steady approach. It works continuously under moisture-retentive dressings, which you'll typically change every few days.
- Enzymatic Debridement: These ointments or solutions need to be applied regularly to keep working, usually once a day.
- Sharp or Conservative Debridement: This is a more hands-on method. You might perform it at each visit, maybe weekly, to clear away any new slough that's appeared and keep things clean.
Your goal is to maintain a clean wound bed that’s ready to heal. That means your debridement schedule should be flexible and based on what you see during your regular assessments.
A good debridement schedule isn't set in stone. It's a living part of the care plan that you adjust based on how the wound is responding. The key is to be consistent in removing that non-viable tissue so the healing process doesn't get stuck in neutral.
What's the Difference Between Slough and Fibrin?
This is a common point of confusion, but getting it right is crucial for proper treatment. Although they can both look yellowish, slough and fibrin are telling you very different stories about what's happening in the wound.
Fibrin is a normal, healthy part of the initial healing cascade. It’s a thin, stringy, whitish-yellow protein that shows up early on to form a sort of scaffold for blood clotting. Slough, on the other hand, is a sign that healing has hit a roadblock. It's a thicker, gunkier mix of dead cells, bacteria, and fluid that can be yellow, tan, or even gray. You want to leave healthy fibrin alone, but slough is always a barrier that needs to go.
Does All Slough Really Need to Be Removed for a Wound to Heal?
Yes, absolutely. For a wound to move out of the inflammatory stage and into the proliferative (healing) stage, that slough has to be cleared out. It acts like a physical wall, literally blocking healthy new granulation tissue from forming.
It also stops epithelial cells from doing their job of migrating across the wound surface to close it up. Removing slough isn't just a suggestion; it’s a core principle of good wound bed preparation and is non-negotiable if you want to see timely, effective healing.
Ready to cut your documentation time by up to 70% and get your entire wound care process running smoothly? Ekagra Health AI is an end-to-end platform that helps with assessments, creates structured charts from your voice notes, and gets you reimbursed faster. Find out how our clinician-designed AI can change your practice at ekagrahealth.ai.

